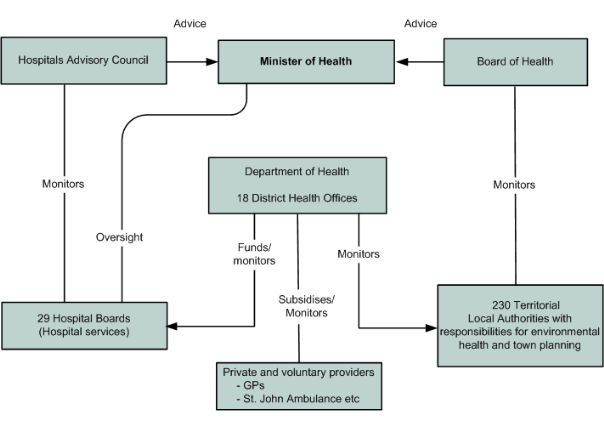
Health Care System
- New Zealand has both public and private health care.
- In the public system, essential health care services such as emergency care, essential surgery and hospital care are provided free for all NZ residents and those living in NZ on a work visa valid for two years or longer.
- Private health care offers treatment of both urgent and non-urgent conditions (excluding A&E). A network of private hospitals and clinics provides a range of services including general surgical procedures and elective procedures.
- Visits to the GP are paid for by the patient.
- The Ministry of Health is responsible for funding and providing state healthcare, which it delegates to District Health Boards (DHBs) whose job is to meet the government’s health objectives by spending their budgets in the most cost-effective way.
- DHBs use their funding to ‘buy’ healthcare services from various ‘suppliers’, including family doctors, hospitals, nursing homes, community-based and non-profit health agencies and private organisations.
ACC Work
The Accident Compensation Corporation (ACC) is the main personal injury insurer in NZ. At one time physiotherapy treatment for claimants was fully reimbursed by ACC, but in November 2009 a new contract came into force.
This has resulted in some changes to practice, where the new policy has sought to limit treatment, for example:
While many of these are positive changes for the benefit of patients, they have also resulted in lower referral and treatment rates by ACC and loss of income, particularly for private practitioners.
However, ACC’s instructions for treatment cannot override ethical or legal principles of patient care, which require patients to be treated to "the maximum practical level".
The Accident Compensation Corporation (ACC) is the main personal injury insurer in NZ. At one time physiotherapy treatment for claimants was fully reimbursed by ACC, but in November 2009 a new contract came into force.
This has resulted in some changes to practice, where the new policy has sought to limit treatment, for example:
- Co-payment - treatment part funded by ACC and part payable by the patient
- Adherence to treatment recommendations in clinical guidelines
- Limits set on permitted number of treatments
- Benchmarking, outcome measurement and quality monitoring of treatment modalities and physiotherapy practice.
While many of these are positive changes for the benefit of patients, they have also resulted in lower referral and treatment rates by ACC and loss of income, particularly for private practitioners.
However, ACC’s instructions for treatment cannot override ethical or legal principles of patient care, which require patients to be treated to "the maximum practical level".